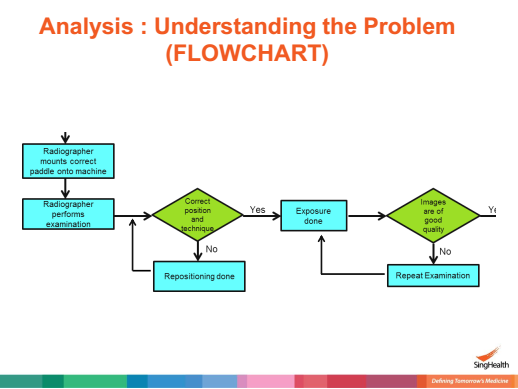
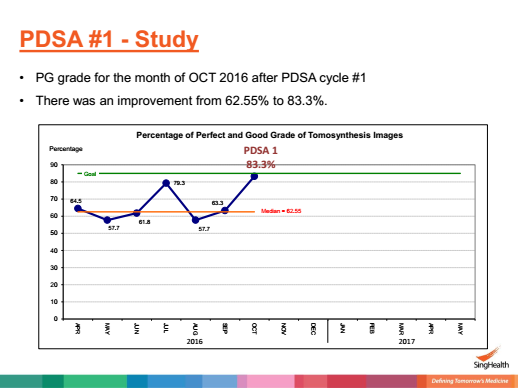
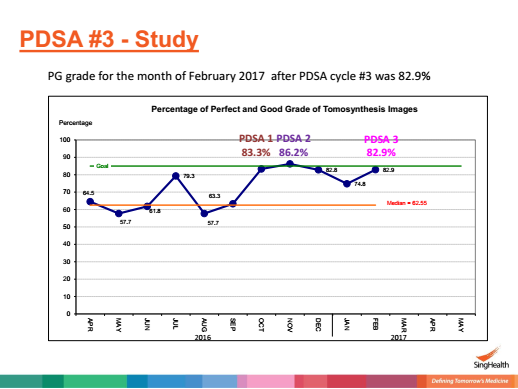
To Improve the Quality of Tomosynthesis Images
| Subject: | 🏥 Health Care |
| Type: | Problem Solution Essay |
| Pages: | 5 |
| Word count: | 1446 |
| Topics: | Breast Cancer, Cancer, Computer Science, Disease, Innovation, Medicine, Nursing |

Need a custom
essay ASAP?
essay ASAP?
We’ll write your essay from scratch and per instructions: even better than this sample, 100% unique, and yours only.
Get essay on this topic
Sources
- Chen, Y. (2007). Digital breast tomosynthesis (DBT): A novel imaging technology to improve early breast cancer detection: implementation, comparison and optimization.
- Jiang, Y., Sahiner, B., Society of Photo-optical Instrumentation Engineers., & American Association of Physicists in Medicine. (2007). Medical imaging 2007: 21-22 February 2007, San Diego, California, USA. Bellingham, Wash: SPIE.
- Nelson, G. S., Fahrig, R., Napel, S., Pelc, N. J., & Stanford University. (2013). Optimization and evaluation of scanning-beam digital X-ray tomosynthesis for real-time 3D image guidance for lung tumor biopsies.
- Philpotts, L. E., & Hooley, R. J. (2016). Breast Tomosynthesis. Saintt Louis: Elsevier Health Sciences.
- Salkowski, L., & Moseley, T. W. (2017). Clinical breast tomosynthesis: A case-based approach to screening and diagnosis. New York: Thieme.
- Sonnenschein, M., & Waldherr, C. (2017). Atlas of breast tomosynthesis: Imaging findings and image-guided interventions. Cham, Switzerland: Springer.
Related Samples
Subject:
💻 Technology
Pages/words: 4 pages/1177 words
Subject:
🧑🤝🧑 Sociology
Pages/words: 1 pages/303 words
Subject:
👸🏽 Famous Person
Pages/words: 3 pages/862 words
Subject:
🌷 Environment
Pages/words: 10 pages/2515 words
Subject:
🏥 Health Care
Pages/words: 4 pages/1036 words
Subject:
🧘🏻 Mental Health
Pages/words: 11 pages/2751 words
Subject:
🏥 Health Care
Pages/words: 2 pages/396 words
Subject:
🏥 Health Care
Pages/words: 3 pages/786 words
Subject:
📡 Media
Pages/words: 3 pages/822 words

Boost your grades with a new guide on A+ writing
Time to excel in writing!
The download will start within seconds.
Download Sample
This essay is publicly available.
Offered for reference purposes only.
Offered for reference purposes only.
By clicking Get this sample, you agree to our Terms & conditions & Privacy policy
Thank you!
The download will start shortly.